Secondary Traumatic Stress: Recognizing & Coping with STS
As a nurse, being exposed to patients’ trauma—whether through direct care or hearing their stories—can have an impact. Secondary Traumatic Stress (STS) is a stress reaction that occurs when a patient’s trauma affects you, even though you weren’t the one who experienced it firsthand (1-6).
STS is a real and valid response to the difficult realities of patient care. Recognizing its signs is the first step toward addressing its impact (1-7).
- You may feel: Jumpy, anxious, or emotionally overwhelmed after hearing about or witnessing trauma. You may struggle with nightmares, avoidance, or difficulty concentrating (5-6, 8).
- Why it matters: STS mimics PTSD, leading to chronic stress, impaired focus, and emotional exhaustion. Left unaddressed, it can impact both patient care and personal well-being (9-10).
References
- Blanco‐Donoso, L. M., Moreno-Jiménez, J., Amutio, A., Gallego-Alberto, L., Moreno‐Jiménez, B., & Garrosa, E. (2020). Stressors, job resources, fear of contagion, and secondary traumatic stress among nursing home workers in face of the COVID-19: the case of Spain. Journal of Applied Gerontology, 40(3), 244–256. https://doi.org/10.1177/0733464820964153
- Ogińska-Bulik, N., Gurowiec, P. J., Michalska, P., & Kȩdra, E. (2021). Prevalence and predictors of secondary traumatic stress symptoms in health care professionals working with trauma victims: A cross-sectional study. PLOS ONE, 16(2), e0247596. https://doi.org/10.1371/journal.pone.0247596
- Rauvola, R. S., Vega, D. M., & Lavigne, K. N. (2019). Compassion Fatigue, Secondary Traumatic Stress, and Vicarious Traumatization: A Qualitative Review and Research Agenda. Occupational Health Science, 3(3), 297–336. https://doi.org/10.1007/s41542-019-00045-1
- Quinn, A., Ji, P., & Nackerud, L. (2018). Predictors of secondary traumatic stress among social workers: Supervision, income, and caseload size. Journal of Social Work, 19(4), 504–528. https://doi.org/10.1177/1468017318762450
- Sprang, G., Ford, J. D., Kerig, P. K., & Bride, B. E. (2019). Defining secondary traumatic stress and developing targeted assessments and interventions: Lessons learned from research and leading experts. Traumatology, 25(2), 72–81. https://doi.org/10.1037/trm0000180
- Marković, M. V., & Živanović, M. (2022). Coping with Secondary Traumatic Stress. International Journal of Environmental Research and Public Health, 19(19), 12881. https://doi.org/10.3390/ijerph191912881
- Fink-Samnick, E. (2022). Collective Occupational Trauma, Health Care Quality, and Trauma-Informed Leadership. Professional Case Management, 27(3), 107–123. https://doi.org/10.1097/ncm.0000000000000559
- Paiva-Salisbury, M. L., & Schwanz, K. A. (2022). Building Compassion Fatigue Resilience: Awareness, Prevention, and Intervention for Pre-Professionals and Current Practitioners. Journal of Health Service Psychology, 48(1), 39–46. https://doi.org/10.1007/s42843-022-00054-9
- Xu, W., Masters, G. A., Simas, T. A. M., Bergman, A. L., & Byatt, N. (2023). Labor and Delivery Clinician perspectives on impact of traumatic clinical experiences and need for systemic supports. Maternal and Child Health Journal, 27(9), 1651–1662. https://doi.org/10.1007/s10995-023-03708-2
- Blanco‐Donoso, L. M., Moreno-Jiménez, J., Amutio, A., Gallego-Alberto, L., Moreno‐Jiménez, B., & Garrosa, E. (2020). Stressors, job resources, fear of contagion, and secondary traumatic stress among nursing home workers in face of the COVID-19: the case of Spain. Journal of Applied Gerontology, 40(3), 244–256. https://doi.org/10.1177/0733464820964153
Where Secondary Traumatic Stress Might Occur
Where can Secondary Traumatic Stress occur?
Secondary Traumatic Stress (STS) occurs when you absorb the trauma of others through patient care—whether by hearing distressing stories, delivering bad news, or witnessing intense emotions (1-4).
High-Risk Situations: STS is more likely in settings with exposure to distressing or traumatic experiences of patients, including:
- Emergency & Trauma Care – Responding to severe injuries and crises.
- Mental Health Services – Supporting patients with past abuse or trauma.
- Pediatrics & Child Welfare – Caring for children affected by neglect or violence.
- Oncology & Palliative Care – Helping patients and families navigate end-of-life realities (1-4).
What Increases Risk?
- Acute or Prolonged Exposure – A single intense event or ongoing trauma exposure can both lead to STS (5-7).
- Personal Vulnerability – Stress or unresolved trauma can heighten susceptibility (4, 8).
- Workplace Culture – Lack of emotional support increases risk (9).
- Limited Training – Those unprepared for trauma-heavy work are more affected (8, 10).
STS is an occupational risk, not a personal weakness. Knowing when and where it happens can help you recognize and manage its effects (9).
- Paiva-Salisbury, M. L., & Schwanz, K. A. (2022). Building Compassion Fatigue Resilience: Awareness, Prevention, and Intervention for Pre-Professionals and Current Practitioners. Journal of Health Service Psychology, 48(1), 39–46. https://doi.org/10.1007/s42843-022-00054-9
- Quinn, A., Ji, P., & Nackerud, L. (2018). Predictors of secondary traumatic stress among social workers: Supervision, income, and caseload size. Journal of Social Work, 19(4), 504–528. https://doi.org/10.1177/1468017318762450
- Ogińska-Bulik, N., Gurowiec, P. J., Michalska, P., & Kȩdra, E. (2021). Prevalence and predictors of secondary traumatic stress symptoms in health care professionals working with trauma victims: A cross-sectional study. PLOS ONE, 16(2), e0247596. https://doi.org/10.1371/journal.pone.0247596
- Marković, M. V., & Živanović, M. (2022). Coping with Secondary Traumatic Stress. International Journal of Environmental Research and Public Health, 19(19), 12881. https://doi.org/10.3390/ijerph191912881
- Cummings, C., Singer, J., Hisaka, R., & Benuto, L. T. (2021). Compassion satisfaction to combat Work-Related burnout, vicarious trauma, and secondary traumatic stress. Journal of Interpersonal Violence, 36(9–10), NP5304–NP5319. https://doi.org/10.1177/0886260518799502
- Mistry, D., Gozna, L., & Cassidy, T. (2021). Psychological and the physical health impacts of forensic workplace trauma. Journal of Forensic Practice, 24(1), 18–33. https://doi.org/10.1108/jfp-05-2021-0027
- Ogińska-Bulik, N., Gurowiec, P. J., Michalska, P., & Kȩdra, E. (2021). Prevalence and predictors of secondary traumatic stress symptoms in health care professionals working with trauma victims: A cross-sectional study. PLOS ONE, 16(2), e0247596. https://doi.org/10.1371/journal.pone.0247596
- Sprang, G., Ford, J. D., Kerig, P. K., & Bride, B. E. (2019). Defining secondary traumatic stress and developing targeted assessments and interventions: Lessons learned from research and leading experts. Traumatology, 25(2), 72–81. https://doi.org/10.1037/trm0000180
- Blanco‐Donoso, L. M., Moreno-Jiménez, J., Amutio, A., Gallego-Alberto, L., Moreno‐Jiménez, B., & Garrosa, E. (2020). Stressors, job resources, fear of contagion, and secondary traumatic stress among nursing home workers in face of the COVID-19: the case of Spain. Journal of Applied Gerontology, 40(3), 244–256. https://doi.org/10.1177/0733464820964153
- Sprang, G., Whitt‐Woosley, A., Wozniak, J., Gusler, S., Hood, C. O., Kinnish, K., & Stroup, H. E. (2023). A Socioecological Approach to Understanding Secondary Trauma in Professionals Working with Survivors of Sex Trafficking: A Hierarchical Regression Analysis. Journal of Interpersonal Violence, 38(21–22), 11745–11767. https://doi.org/10.1177/08862605231188047
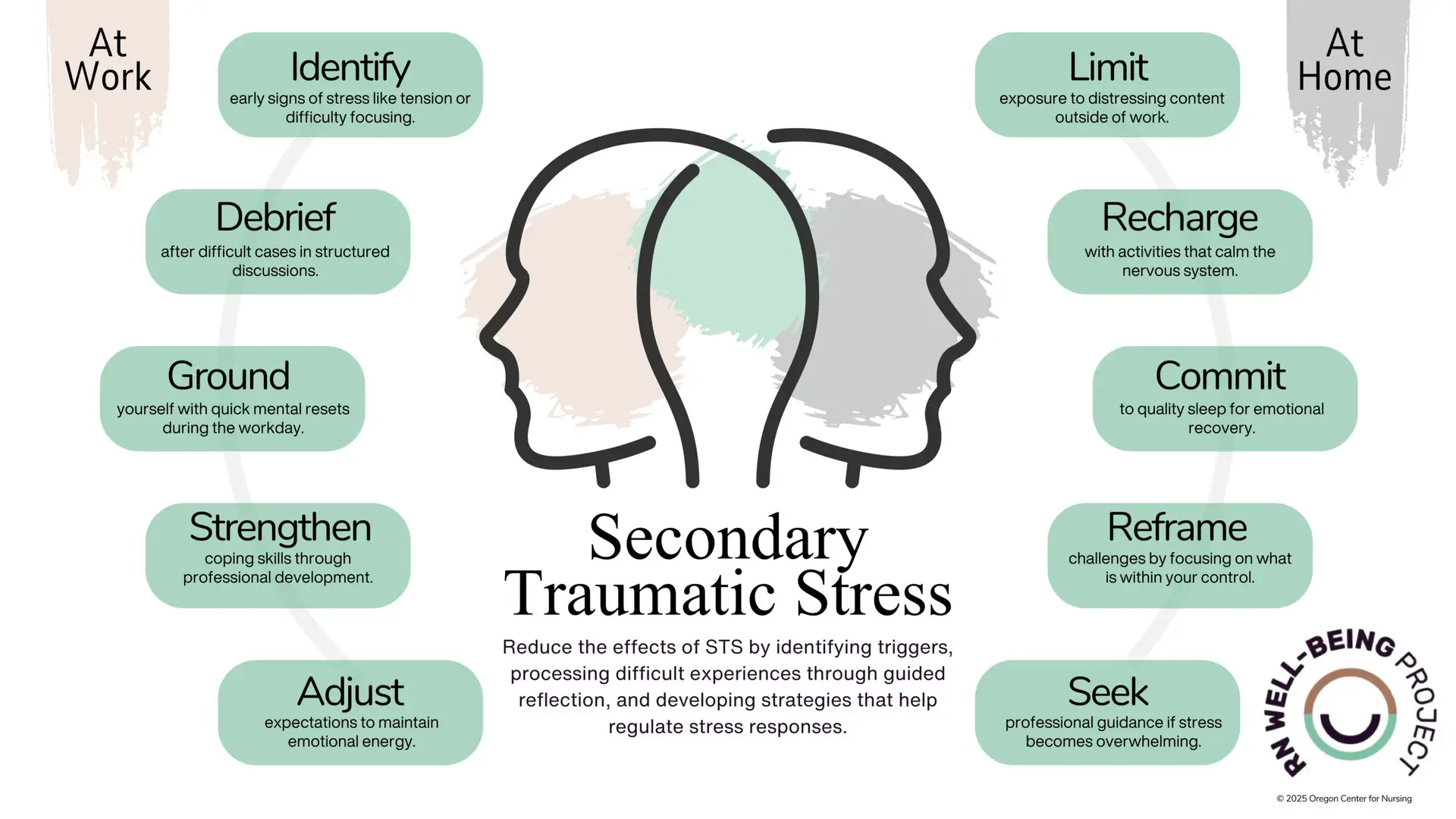
How can I manage Secondary Traumatic Stress at work?
STS can make it harder to stay present, connect with patients, or feel a sense of purpose at work. While the nature of the job won’t change, your approach to handling stress can. These strategies help manage STS in ways that fit into your daily routine:
- Anchor Yourself in the Moment – Short mindfulness exercises or breathwork between tasks can help regulate stress (1).
- Shift How You Process Stress – When difficult situations arise, notice your reaction and work on reframing thoughts to prevent emotional overload (2).
- Turn to Trusted Colleagues – Connecting with coworkers who understand the weight of the job can help reduce feelings of isolation (3).
- Recognize Growth in Challenges – Engaging in professional development or reflecting on meaningful moments can reinforce a sense of purpose.
- Protect Your Energy – Set limits on overextending yourself, take regular breaks, and be intentional about maintaining time away from work.
- Paiva-Salisbury, M. L., & Schwanz, K. A. (2022). Building Compassion Fatigue Resilience: Awareness, Prevention, and Intervention for Pre-Professionals and Current Practitioners. Journal of Health Service Psychology, 48(1), 39–46. https://doi.org/10.1007/s42843-022-00054-9
- Marković, M. V., & Živanović, M. (2022). Coping with Secondary Traumatic Stress. International Journal of Environmental Research and Public Health, 19(19), 12881. https://doi.org/10.3390/ijerph191912881
- Ogińska-Bulik, N., Gurowiec, P. J., Michalska, P., & Kȩdra, E. (2021). Prevalence and predictors of secondary traumatic stress symptoms in health care professionals working with trauma victims: A cross-sectional study. PLOS ONE, 16(2), e0247596. https://doi.org/10.1371/journal.pone.0247596
How can I manage Secondary Traumatic Stress at home?
STS doesn’t stay at work—it can follow you home, affecting your mood, relationships, and overall well-being. Making time for activities that restore your energy and mindset can help prevent it from taking over your personal life.
- Build a Routine That Grounds You – Regular movement, balanced meals, and consistent sleep habits help strengthen emotional resilience (1).
- Prioritize Rest That Actually Restores You – Quality sleep is essential for emotional regulation, so create a bedtime routine that supports deep, uninterrupted sleep (2).
- Find What Calms Your Mind – Activities like yoga, spending time in nature, or guided relaxation exercises can reduce anxiety and improve mental well-being.
- Stay Connected to People Who Get You – Talking to trusted friends or family members can help process difficult experiences and prevent isolation (3).
- Recognize When Extra Support is Needed – If stress feels overwhelming, seeking professional help can provide tools to navigate it more effectively (4).
- Choose Coping Strategies That Support Recovery – Processing difficult experiences in a healthy way can reduce the impact of STS. Strategies like reframing challenges, focusing on what you can control, and accepting what cannot be changed can help build resilience (3-5).
- Avoid Unhealthy Coping Mechanisms – Some strategies may feel like relief in the moment but can worsen STS over time. Substance use, emotionally shutting down, or mentally disconnecting from the issue can make it harder to process stress and may lead to more distress in the long run (3, 5).
- Quinn, A., Ji, P., & Nackerud, L. (2018). Predictors of secondary traumatic stress among social workers: Supervision, income, and caseload size. Journal of Social Work, 19(4), 504–528. https://doi.org/10.1177/1468017318762450
- Xie, W., Wang, J., Okoli, C. T., He, H., Feng, F., Zhuang, L., Tang, P., Zeng, L., & Jin, M. (2020). Prevalence and factors of compassion fatigue among Chinese psychiatric nurses. Medicine, 99(29), e21083. https://doi.org/10.1097/md.0000000000021083
- Ogińska-Bulik, N., Gurowiec, P. J., Michalska, P., & Kȩdra, E. (2021). Prevalence and predictors of secondary traumatic stress symptoms in health care professionals working with trauma victims: A cross-sectional study. PLOS ONE, 16(2), e0247596. https://doi.org/10.1371/journal.pone.0247596
- Marsac, M. L., & Ragsdale, L. B. (2020). Tips for recognizing, managing secondary traumatic stress in yourself. AAP News. https://www.aappublications.org/news/2020/05/21/wellness052120
- Marković, M. V., & Živanović, M. (2022). Coping with Secondary Traumatic Stress. International Journal of Environmental Research and Public Health, 19(19), 12881. https://doi.org/10.3390/ijerph191912881
How can I build on post-traumatic growth?
Experiencing Secondary Traumatic Stress (STS) can be overwhelming, but it doesn’t have to define your career. Many healthcare professionals find that facing these challenges leads to personal and professional growth—known as post-traumatic growth (PTG). This can mean discovering new strengths, deepening empathy, or gaining a renewed sense of purpose in your work (1-2).
Rebuilding Meaning and Purpose
- Find the “Why” in Your Work – STS can make it easy to focus on hardship, but reflecting on moments of impact—when you made a real difference for a patient or family—can help reinforce your sense of purpose (2).
- Shift Perspective – Instead of seeing STS as something that only takes from you, consider how it has added to your professional and personal strength. Have you become more patient? A better listener? More confident under pressure? Acknowledging these changes can help reframe your experience (1).
Strengthening Emotional Endurance
- Turn Reflection into Action – Writing down or talking through what you’ve learned from difficult cases can help you identify patterns, recognize what is within your control, and refine how you respond to emotional strain (2).
- Embrace Support Networks – STS can feel isolating, but sharing experiences with colleagues, mentors, or peer support groups can normalize your feelings and provide strategies to move forward (1).
- Keep Learning and Adapting – Trauma exposure changes you—but how it changes you is something you can influence. Engaging in continued education, training in trauma-informed care, or professional debriefing can help transform stress into growth (2).
Growth after STS doesn’t mean ignoring the difficulties—it means using them to build emotional resilience and a stronger sense of self. By shifting your mindset, leaning into support, and finding meaning in your experiences, you can move forward with a renewed capacity to care for both your patients and yourself.
STS is a natural response to the emotional intensity of patient care. It can affect both the mind and body, leading to hypervigilance, emotional withdrawal, or difficulty concentrating. While these reactions can feel isolating, they are not personal failures. With the right strategies—such as structured debriefing, professional support, and intentional recovery—nurses can manage STS while continuing to provide high-quality care.
- Moreno-Jiménez, J. E., Blanco-Donoso, L. M., Demerouti, E., Belda Hofheinz, S., Chico-Fernández, M., Moreno-Jiménez, B., & Garrosa, E. (2021). The Role of Healthcare Professionals’ Passion in Predicting Secondary Traumatic Stress and Posttraumatic Growth in the Face of COVID-19: A Longitudinal Approach. International Journal of Environmental Research and Public Health, 18(9), 4453. https://doi.org/10.3390/ijerph18094453
- Tsirimokou, A., Kloess, J. A., & Dhinse, S. K. (2023). Vicarious Post-traumatic Growth in Professionals Exposed to Traumatogenic Material: A Systematic Literature Review. Trauma, Violence, & Abuse, 24(3), 1848–1866. https://doi.org/10.1177/15248380221082079
STS is a natural response to the emotional intensity of patient care. It can affect both the mind and body, leading to hypervigilance, emotional withdrawal, or difficulty concentrating. While these reactions can feel isolating, they are not personal failures. With the right strategies—such as structured debriefing, professional support, and intentional recovery—nurses can manage STS while continuing to provide high-quality care.