Vicarious Trauma: Understanding & Managing the Impact
Vicarious trauma stems from prolonged exposure to others’ traumatic experiences, particularly when an individual deeply engages with these stories. This prolonged exposure can lead to enduring changes in the individual’s own emotional and psychological experiences. It manifests as disruptions and shifts in their beliefs about themselves, their relationships, and their understanding of the world (1-5).
- You may feel: A shift in how you see yourself, others, or the world—leading to loss of trust, safety, or meaning. You may withdraw, struggle with intrusive thoughts, or experience emotional numbness (1-3).
- Why it matters: VT can cause lasting emotional and psychological changes, making it harder to connect with patients, maintain healthy relationships, and feel fulfilled in your work (6-8).
References
- Rauvola, R. S., Vega, D. M., & Lavigne, K. N. (2019). Compassion Fatigue, Secondary Traumatic Stress, and Vicarious Traumatization: a Qualitative Review and Research Agenda. Occupational Health Science, 3(3), 297–336. https://doi.org/10.1007/s41542-019-00045-1
- Fink-Samnick, E. (2022). Collective Occupational Trauma, Health Care Quality, and Trauma-Informed Leadership. Professional Case Management, 27(3), 107–123. https://doi.org/10.1097/ncm.0000000000000559
- Isobel, S., & Thomas, M. (2021). Vicarious trauma and nursing: An integrative review. International Journal of Mental Health Nursing, 31(2), 247–259. https://doi.org/10.1111/inm.12953
- Kennedy, S., & Booth, R. (2022). Vicarious trauma in nursing professionals: A concept analysis. Nursing Forum, 57(5), 893–897. https://doi.org/10.1111/nuf.12734
- Ogińska-Bulik, N., Gurowiec, P. J., Michalska, P., & Kȩdra, E. (2021). Prevalence and predictors of secondary traumatic stress symptoms in health care professionals working with trauma victims: A cross-sectional study. PLOS ONE, 16(2), e0247596. https://doi.org/10.1371/journal.pone.0247596
- Cummings, C., Singer, J., Hisaka, R., & Benuto, L. T. (2021). Compassion satisfaction to combat Work-Related burnout, vicarious trauma, and secondary traumatic stress. Journal of Interpersonal Violence, 36(9–10), NP5304–NP5319. https://doi.org/10.1177/0886260518799502
- Roberts, C., Darroch, F., Giles, A. R., & Van Bruggen, R. (2022). You’re carrying so many people’s stories: vicarious trauma among fly-in fly-out mental health service providers in Canada. International Journal of Qualitative Studies on Health and Well-being, 17(1). https://doi.org/10.1080/17482631.2022.2040089
- Sprang, G., Ford, J. D., Kerig, P. K., & Bride, B. E. (2019). Defining secondary traumatic stress and developing targeted assessments and interventions: Lessons learned from research and leading experts. Traumatology, 25(2), 72–81. https://doi.org/10.1037/trm0000180
Where can Vicarious Trauma occur?
Vicarious trauma in healthcare can occur in various scenarios, often when healthcare professionals are exposed to the suffering, trauma, or distress of their patients. Some common places where vicarious trauma can occur:
- End-of-Life & Hospice Care – Frequent exposure to witnessing the suffering and eventual death of patients (1-5).
- Pediatrics, Veterans, & Abuse Survivors – Providing care for vulnerable populations can be emotionally taxing, particularly when their experiences of trauma intersect with their healthcare needs (2-3).
- Emergency, Trauma & Mental Health Units – High exposure to crisis situations, severe injuries, and psychiatric distress (3-5).
- Oncology & Chronic Illness Clinics – Witnessing prolonged suffering and limited treatment options (2, 4).
- Disaster & Mass Casualty Response – Large-scale emergencies amplify emotional strain (3).
- Lack of Workplace Support – Healthcare professionals who feel isolated or unsupported by their colleagues, supervisors, or organizations may be more vulnerable to the negative effects of vicarious trauma (3, 5).
- Ogińska-Bulik, N., Gurowiec, P. J., Michalska, P., & Kȩdra, E. (2021). Prevalence and predictors of secondary traumatic stress symptoms in health care professionals working with trauma victims: A cross-sectional study. PLOS ONE, 16(2), e0247596. https://doi.org/10.1371/journal.pone.0247596
- Kennedy, S., & Booth, R. (2022). Vicarious trauma in nursing professionals: A concept analysis. Nursing Forum, 57(5), 893–897. https://doi.org/10.1111/nuf.12734
- Isobel, S., & Thomas, M. (2021). Vicarious trauma and nursing: An integrative review. International Journal of Mental Health Nursing, 31(2), 247–259. https://doi.org/10.1111/inm.12953
- Fink-Samnick, E. (2022). Collective Occupational Trauma, Health Care Quality, and Trauma-Informed Leadership. Professional Case Management, 27(3), 107–123. https://doi.org/10.1097/ncm.0000000000000559
- Roberts, C., Darroch, F., Giles, A. R., & Van Bruggen, R. (2022). You’re carrying so many people’s stories: vicarious trauma among fly-in fly-out mental health service providers in Canada. International Journal of Qualitative Studies on Health and Well-being, 17(1). https://doi.org/10.1080/17482631.2022.2040089
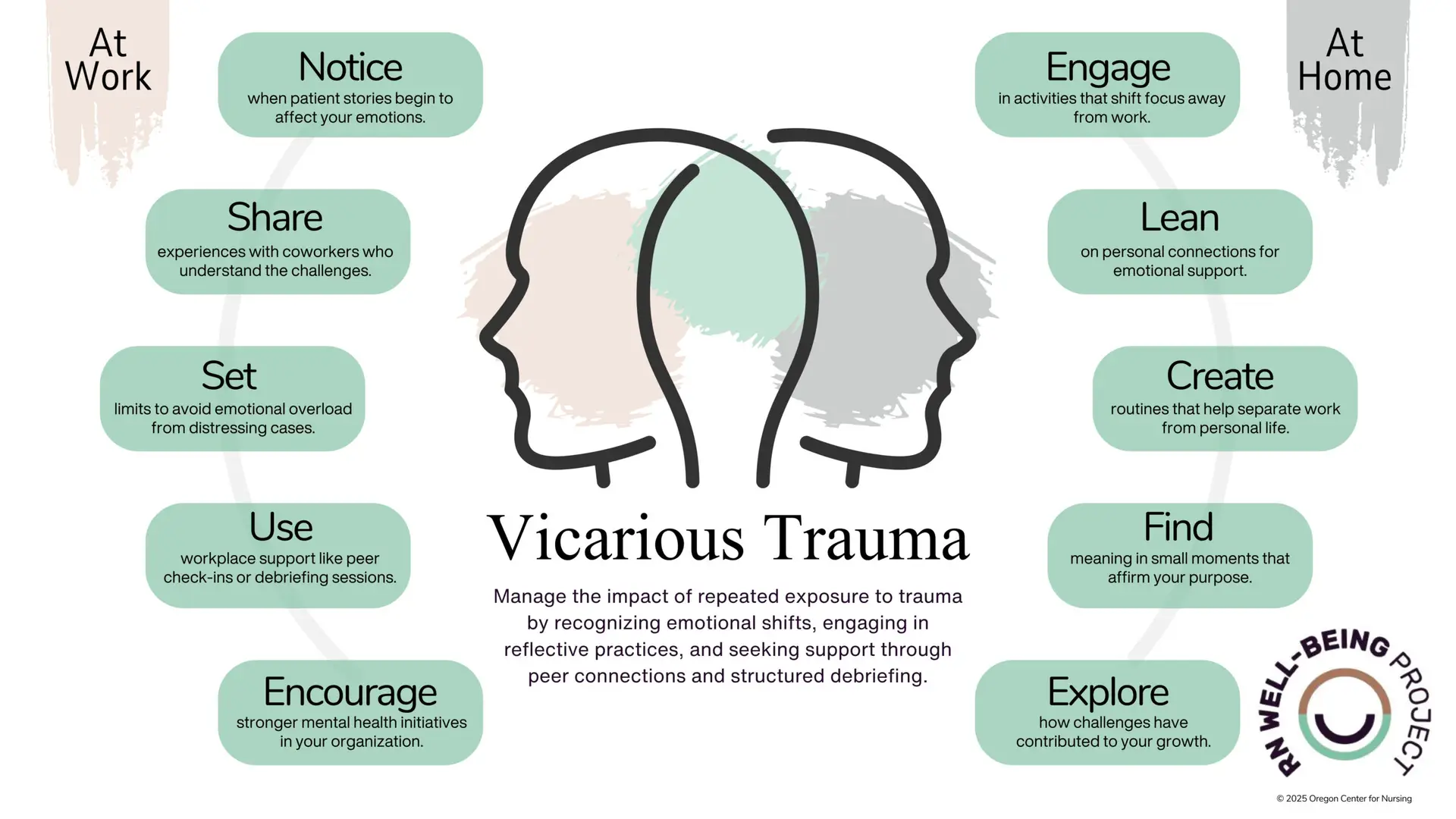
How do I manage Vicarious Trauma at work?
Managing vicarious trauma requires both individual strategies and systemic support (1). Here’s what you can do:
- Check in with Yourself: Pay attention to how you’re feeling and recognize when work is taking an emotional toll. Self-reflection can help you understand your triggers and manage their impact (2-3).
- Talk About It: Don’t keep difficult experiences bottled up. Share your thoughts with trusted colleagues, friends, or mentors—it helps process emotions and normalizes open conversations about vicarious trauma (2).
- Set Boundaries That Work for You: Know where to draw the line between work and personal life. Protecting your emotional space doesn’t mean you care less—it helps you stay present and effective (2, 4).
- Lean on Your Team: Build strong connections with coworkers who understand the challenges. A solid support network can make tough days more manageable (2-3).
- Use Workplace Resources: If debriefing, mental health support, or peer groups are available, take advantage of them. If they aren’t, ask leadership what options exist (2, 3).
- Speak Up for System-Wide Change: If you see gaps in workplace support, team up with colleagues to push for better policies, like training programs or balanced workloads. Small changes can make a big difference (2, 4).
- Fink-Samnick, E. (2022). Collective Occupational Trauma, Health Care Quality, and Trauma-Informed Leadership. Professional Case Management, 27(3), 107–123. https://doi.org/10.1097/ncm.0000000000000559
- Isobel, S., & Thomas, M. (2021). Vicarious trauma and nursing: An integrative review. International Journal of Mental Health Nursing, 31(2), 247–259. https://doi.org/10.1111/inm.12953
- Roberts, C., Darroch, F., Giles, A. R., & Van Bruggen, R. (2022). You’re carrying so many people’s stories: vicarious trauma among fly-in fly-out mental health service providers in Canada. International Journal of Qualitative Studies on Health and Well-being, 17(1). https://doi.org/10.1080/17482631.2022.2040089
- Kennedy, S., & Booth, R. (2022). Vicarious trauma in nursing professionals: A concept analysis. Nursing Forum, 57(5), 893–897. https://doi.org/10.1111/nuf.12734
How do I manage Vicarious Trauma at home?
- Make Time for What Brings You Joy – Engage in activities that help you decompress—whether it’s art, music, laughter, or simple stress-relief practices (1-2).
- Lean on Your Support System – Talk to trusted friends, family, or professionals when you’re feeling overwhelmed. Support from others can help ease emotional strain (1-2).
- Create Space Between Work and Personal Life – Prioritize time for yourself outside of work—through hobbies, relaxation, or being with loved ones—to maintain emotional well-being (1).
- Reframe Challenges When Possible – Finding small positives or focusing on what’s within your control can help strengthen resilience in difficult moments (2).
- Isobel, S., & Thomas, M. (2021). Vicarious trauma and nursing: An integrative review. International Journal of Mental Health Nursing, 31(2), 247–259. https://doi.org/10.1111/inm.12953
- Roberts, C., Darroch, F., Giles, A. R., & Van Bruggen, R. (2022). You’re carrying so many people’s stories: vicarious trauma among fly-in fly-out mental health service providers in Canada. International Journal of Qualitative Studies on Health and Well-being, 17(1). https://doi.org/10.1080/17482631.2022.2040089
How do I grow through Vicarious Resilience?
Not all exposure to trauma leads to distress—vicarious resilience is the ability to find strength, meaning, and personal growth through the challenges you witness in your work. Instead of just enduring difficult moments, you can learn from them and use them to build emotional resilience (1).
Ways to Strengthen Vicarious Resilience
- Recognize Your Own Growth: Take note of how you’ve developed professionally and emotionally through your experiences. Acknowledge the skills, empathy, and insight you’ve gained along the way.
- Keep Learning: Trauma-informed training and resilience-building strategies can help you navigate difficult situations while also protecting your emotional well-being.
- Stay Connected: Whether it’s through a quick conversation with a colleague or a deeper discussion with a mentor, sharing experiences with people who understand can be a source of strength.
- Take Advantage of Available Support: If your workplace offers counseling, peer support groups, or debriefing sessions, consider participating. Seeking support is an investment in yourself.
- Focus on the Meaning in Your Work: The care you provide has real impact. Holding onto the purpose behind what you do can help you find fulfillment even in the toughest moments.
Rauvola, R. S., Vega, D. M., & Lavigne, K. N. (2019). Compassion Fatigue, Secondary Traumatic Stress, and Vicarious Traumatization: a Qualitative Review and Research Agenda. Occupational Health Science, 3(3), 297–336. https://doi.org/10.1007/s41542-019-00045-1
Vicarious trauma is an occupational risk that can reshape the way nurses view their work, relationships, and sense of safety. Recognizing these emotional shifts and taking intentional steps to restore balance can help sustain a fulfilling nursing career. In addition, developing awareness, setting boundaries, and engaging in self-restoration allow nurses to remain present in their work without being consumed.