Manageable Stressor: Vicarious Trauma
The lasting impact of repeated exposure to patient trauma.
Nurses bear witness to some of the most profound moments in a patient’s life—often the hardest ones. Over time, repeated exposure to suffering, tragedy, and distress can leave a mark. Vicarious trauma is not just about witnessing pain; it’s about how that exposure can gradually reshape a nurse’s worldview, sense of self, and emotional well-being.
What is Vicarious Trauma?
Vicarious trauma is a persistent psychological shift that develops over time as a result of ongoing exposure to the trauma of others. Unlike acute stress reactions that fade, vicarious trauma accumulates, leading to changes in a nurse’s sense of safety, trust, esteem, control, and identity.
This is not burnout. It is a fundamental change in how a person processes the world due to prolonged exposure to trauma. Left unaddressed, it can impact a nurse’s ability to engage with work, maintain well-being, and provide compassionate care [1-7].
Recognizing Vicarious Trauma
Vicarious trauma isn’t always obvious, but it shows up in patterns of behavior, emotional shifts, and physical symptoms. It can develop in any healthcare setting, especially where staff regularly witness patient suffering—such as emergency care, palliative care, mental health, pediatrics, and disaster response. Employers should watch for:
- Workplace Signs: Absenteeism, disengagement, declining performance [3].
- Behavioral Changes: Withdrawal, isolation, cynicism, trouble focusing [3,4].
- Emotional Shifts: Anxiety, numbness, sadness, shame [3, 5].
- Physical Symptoms: Fatigue, sleep issues, tachycardia [3].
Spotting these changes early can help identify when staff may be struggling with vicarious trauma.
Preventing & Addressing Vicarious Trauma
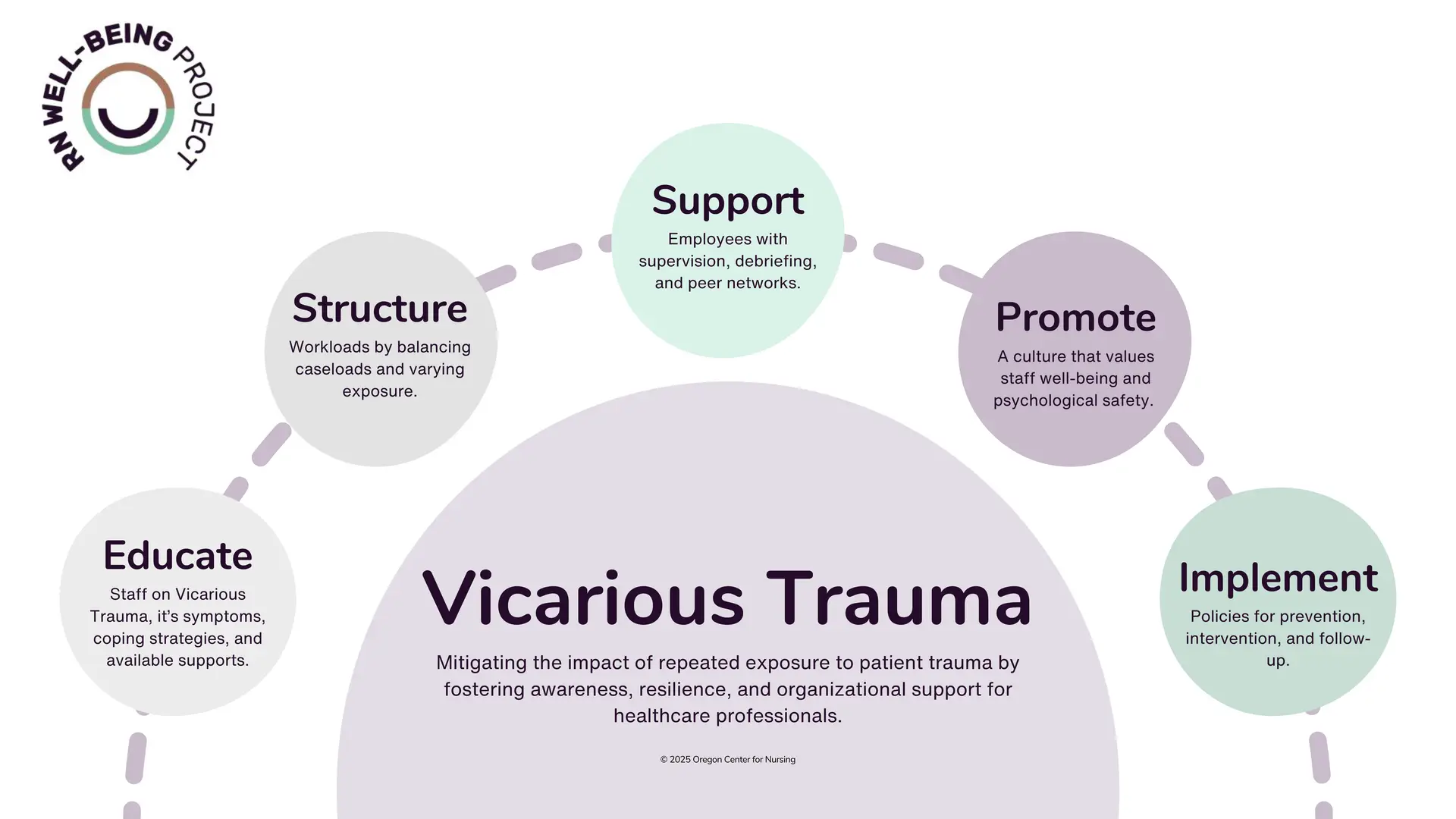
Vicarious trauma can’t be eliminated, but organizations can take proactive steps to reduce its impact. Prevention starts with education, workload management, and a supportive culture. When VT does occur, structured support systems can help staff recover.
Preventing & Addressing Vicarious Trauma
- Tailored Education & Training: Provide targeted training on VT recognition, coping strategies, and resilience-building [3, 6, 5].
- Workload Management: Implement case management strategies to balance caseloads and reduce the risk of VT [3, 6, 5].
- Supportive Culture: Foster open conversations about VT and create an environment where seeking help is encouraged [3, 5].
- Clear Policies: Develop guidelines for prevention, screening, and intervention to ensure a structured approach [3, 5].
Supporting Affected Staff
- Systemic Support: Offer clinical supervision and structured debriefing sessions after difficult [3, 6, 5].
- Mental Health Resources: Ensure access to counseling, peer support, and professional development on resilience [3, 6, 5].
- Retention & Growth: Provide opportunities for staff to process experiences, reframe challenges, and find fulfillment in their work [6].
References
[1] Rauvola, R. S., Vega, D. M., & Lavigne, K. N. (2019). Compassion Fatigue, Secondary Traumatic Stress, and Vicarious Traumatization: a Qualitative Review and Research Agenda. Occupational Health Science, 3(3), 297–336. https://doi.org/10.1007/s41542-019-00045-1
[2] Fink-Samnick, E. (2022). Collective Occupational Trauma, Health Care Quality, and Trauma-Informed Leadership. Professional Case Management, 27(3), 107–123. https://doi.org/10.1097/ncm.0000000000000559
[3] Isobel, S., & Thomas, M. (2021). Vicarious trauma and nursing: An integrative review. International Journal of Mental Health Nursing, 31(2), 247–259. https://doi.org/10.1111/inm.12953
[4] Mistry, D., Gozna, L., & Cassidy, T. (2021). Psychological and the physical health impacts of forensic workplace trauma. Journal of Forensic Practice, 24(1), 18–33. https://doi.org/10.1108/jfp-05-2021-0027
[5] Kennedy, S., & Booth, R. (2022). Vicarious trauma in nursing professionals: A concept analysis. Nursing Forum, 57(5), 893–897. https://doi.org/10.1111/nuf.12734
[6] Roberts, C., Darroch, F., Giles, A. R., & Van Bruggen, R. (2022). You’re carrying so many people’s stories: vicarious trauma among fly-in fly-out mental health service providers in Canada. International Journal of Qualitative Studies on Health and Well-being, 17(1). https://doi.org/10.1080/17482631.2022.2040089
[7] Sprang, G., Ford, J. D., Kerig, P. K., & Bride, B. E. (2019). Defining secondary traumatic stress and developing targeted assessments and interventions: Lessons learned from research and leading experts. Traumatology, 25(2), 72–81. https://doi.org/10.1037/trm0000180